|
Wisdom Teeth Extraction
The information presented on this site is of personal opinion and consequently is slanted and biased and not based on proper scientific research. The information presented is NOT written by a dental expert. Further the information presented has NOT been subjected to peer review by experts to verify accuracy and data integrity.
Refer to the wisdom teeth page for a discussion of the reasons and indications for having a wisdom tooth removed. Controversy exists surrounding whether healthy disease free wisdom teeth should be removed. 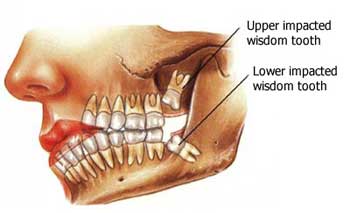
It has been shown by some health care institution audits that 18% to 60% of patients have had their wisdom teeth removed for preventative reasons - controversial. [11-13]
If you must get your wisdom teeth removed ask your dentist and oral surgeon why it is necessary and, if you are not satisfied with the answer, get a second and possibly even a third opinion. You should consider having an oral surgeon remove any wisdom tooth instead of your dentist. You may also consider having surgery done at a hospital.
If you live in the U.S. understand that the current legal system has many issues. See this page on the U.S. legal system and medical malpractice for explanation.
What happens before surgery?
Your dentist may refer you to an oral surgeon and provide you with your panoramic x-rays to bring to the oral surgeon. Before a wisdom tooth is removed you will have what is known as a consultation which typically lasts between 20 to 30 minutes. Some oral surgeons prefer to have the consultation directly before any wisdom teeth are extracted whereas other oral surgeons prefer to have the consultation on a seperate day. You and your oral surgeon will review your x-rays and the oral surgeon will go over some of the complications that could potentially occur. If you had any additional imaging studies such as cone beam CT-scan (CBCT) or you wish to have CBCT done or your surgeon recommends CBCT this will also be reviewed and/or discussed.
You and your surgeon will need to decide what kind of anaesthetic to use of which there are typically 4 options.
1) Most people have a local anaesthetic. This is an injection that numbs part of your mouth. It’s the same painkiller you might have had for a filling. You’ll need two or three injections into your gum. It works for the length of the operation: about 40 minutes. But your lip or tongue will still feel numb two or three hours after. Having only local anesthesia has the least amount of potential complications that can occur.
2) Some people have have nitrous oxide and oxygen which is known as laughing gas although this makes you aware of what is going on. This will be in combination with a local anesthetic.
3) Some people have conscious sedation also known as IV sedation in combination with local anesthesia. A sedative drug is fed through a needle into the back of your hand or arm. You could also be given a pill, but this isn’t as common. You’ll feel very relaxed and sleepy, but you’ll still be awake. You won’t feel any pain.
4) Some people have a general anaesthetic. This makes you sleep and remain unconscious. There are more risks with a general anaesthetic than a local anaesthetic. General anesthesia is normally only given in a hospital by an anesthesiologist.
Depending on what option you select for your anaesthetic and/or sedative(s) you may need to not eat and not drink anything prior to surgery for at least 6 to 8 hours (typical with option 3 and 4 above). This is because anesthesia that is given when someone has recently eaten could cause them to vomit and throw up which could be life threatening.
I encourage you to learn more in depth about the differences between anaesthesia and sedation as you have a potential choice and input in the medications received.
Your surgeon will provide you with a consent form and ask you to read it and sign it. Instructions for the procedure and any prescriptions may be given as well.
The cost for the procedure and forms of payment will also be discussed.
If you are looking for an example of a consent form or to know an estimate of the cost click the links.
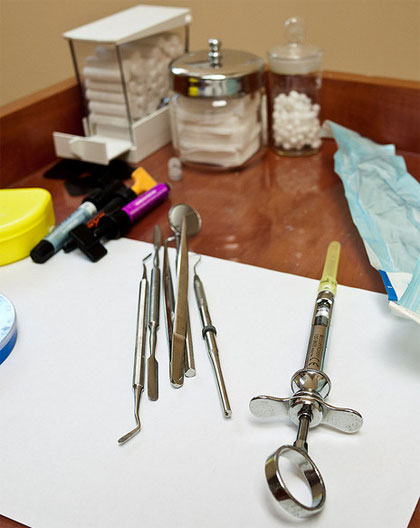
This image is from http://www.flickr.com/photos/secgeek/4294708744/. It is used with permission.
What happens during surgery?
Removing all four wisdom teeth lasts 20 to 30 minutes in a skilled surgeon. This time increases based on the experience, staff support, and type of instruments the surgeon has access to. It could take up to an hour if you’re having all four teeth removed or if the wisdom teeth are difficult to extract. The longer the operation lasts the greater the risk of complications occuring.
Here’s what happens.
• Your surgeon will usually make a small cut into your gum to get to the tooth underneath.
• Then, he or she will sometimes remove bone around the tooth and take out the tooth. A drill is usually used, but sometimes the operation is done with a small chisel.
• Depending on the position of the tooth, your dentist or surgeon may need to cut the tooth into pieces to make it easier to take out. A saltwater spray is put into your mouth to wash away blood and bits of tooth.
• Once the tooth is removed, your surgeon will stitch your gum back up using stitches that will dissolve or may require removal, depending on their preference.
How well does the operation work?
Your wisdom teeth will not grow back. If you haven't yet checked out the complications, please do so. It is possible to have your overall quality of life reduced after having a wisdom tooth removed if you suffer a complication. If you had problems with a wisdom tooth or wisdom teeth prior to surgery it is possible to have your quality of life improved.
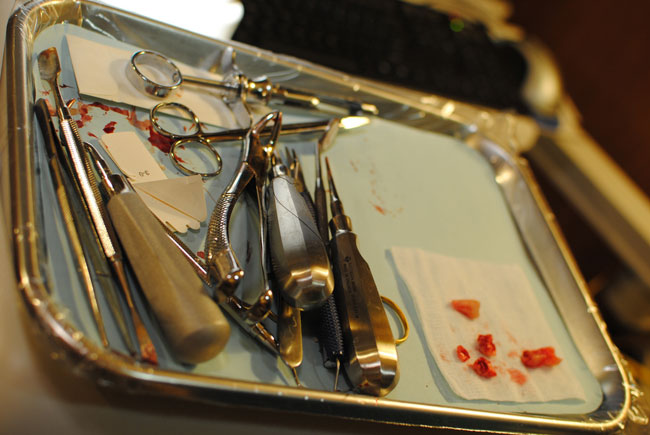
This image is from http://www.flickr.com/photos/gbullard/4709219583/ and has a Creative Commons License. It is used with permission.
Post Operative Advice
Post operative advice varies from oral surgeon to oral surgeon and depending on which source one looks at. Therefore, the following advice is meant to serve as a general guide.
Immediately After Surgery
Sit still for a few minutes immediately after surgery because you want to be sure that a blood clot has formed. Then you will often walk a few steps with the aid of an assistant to a recovery room. There you will rest for some time which could be up to 30 minutes or an hour if you tend to bleed longer than most people.You will generally sit still for at least 20 minutes after surgery. You will bite on gauze while you are waiting to keep pressure on the site and stop the bleeding.
If you had IV sedation or general anesthesia you will need someone to drive you home.
After you leave the office, you should be somewhat still and not do anything strenuous. Don’t suck or spit, as this will stop the formation of a blood clot which is needed to prevent dry socket. Bleeding is normal but if you notice thick bleeding with dark red blood clots, you need to apply more pressure (you can use your fingers). Use either gauze or a paper towel and wad it up so it puts pressure directly on the site. You should change the gauze every 15 - 45 minutes until bleeding stops. You may also use a moistened tag and apply pressure to it if gauze is not successful in stopping bleeding. If bleeding continues to persist contact your surgeon and don't hesitate to go to the hospital emergency room.
Pain
The pain usually peaks three hours to six hours after the operation and remains elevated for several days. Pain normally goes away after five days to ten days. You’ll need to take painkillers at first such as over the counter drugs you can buy at the pharmacy: aspirin (Bayer), ibuprofen (Advil) or acetaminophen (Tylenol). You may be prescribed a narcotic such as codeine, vicodin, or perocet of which you (or someone on your behalf) will need to bring a prescription to the pharmacy. You may want to take painkillers regularly for the first few days, and only when you feel you need them after that. Medications have side effects so make sure you read any instructions and precautions. If you experience any nausea from surgery you may want to not start any potential narcotics untill it has subsided (nausea may be helped to subside by drinking carbonated water, ginger ale, 7UP, ginger tea, or taking an anti-nausea medication). Besure to discuss any concerns you may have with your pain medications with your doctor, surgeon, and/or pharmacist.
Swelling
Use ice packs to help control swelling. 10-20 minutes on followed by 10-20 minutes off of applying ice will help reduce swelling and minimize pain. Swelling typically remains elevated for a few days. Three days after surgery you can replace ice with moist heat to the sides of the face. This reduces swelling and increases the range of motion of your jaw. However, do not apply any heat where swelling occurs that is due to an infection.
Mouth Rinse/Brushing
The day after surgery, rinse your mouth gently with warm salt water or warm tap water at least six times a day. Mix 1/2 teaspoon of table salt in 8 ounces of water. Be very gentle when brushing your teeth around the area where surgery was. There will be a socket or a cavity (as in a hole - not a dental carie) where the tooth was removed. This area will gradually fill in with the new tissue over the next month and it is important to keep it clean. Make sure you do not rinse or brush on the evening of your surgery and instead start the following day. You can continue rinsing for up to 14 days.
Diet
Drink a lot of clear liquids and only eat soft foods for at least the first few days (preferably near a week). Be sure you avoid hard or crunchy foods, such as popcorn and hard candy, for at least two weeks after surgery. Make sure you drink plenty of fluids (8 glasses of water) to prevent dehyrdration. Avoid hot liquids and alcohol for the first day.
If you are looking for more information on what to eat after wisdom teeth removal click the link.
Returning too quickly to a normal diet could lead to a lower jaw fracture (mandible fracture). Men tend to have greater biting forces than women which could lead them to develop more mandibular fractures. As one ages the mandible weakens due to reduction in bony elasticity. These and other high risk groups (deep bony impaction, pathology present) for mandibular fracture should consider being on a restricted soft diet for at least 4 weeks after surgery as a preventative measure. [8]
Physical Activity
You will want to take it easy and get plenty of rest. You should avoid doing anything strenuous for the first few days to prevent bleeding and to prevent any sutures (stiches) from reopening. After three days you can begin to ease back into some physical activity.
Follow-up Appointment
Typically you will set up a follow-up appointment with your surgeon which is five to seven days after the surgery. This appointment usually only lasts several minutes and allows for the surgeon to inspect any extraction site(s) to establish if healing is properly occuring and remove any potential sutures (stiches).
Some oral surgeons offer the ability for a follow up appointment to occur via phone or email although the majority of follow up appointments are office visits. Hence it is possible to see an oral surgeon only once for wisdom teeth removal as the consultation, surgery, and dissolvable sutures (stiches) can be placed all in the same day. [6, 9]
This website's owner personally recommends seing your oral surgeon on three different occasions for the consultation, surgery, and follow-up appointment as it may help reduce anxiety and allow for questions to be addressed.
Updated December 16, 2011
References
1. Removing Wisdom Teeth. Clinical Evidence, the British Medical Journal. Written September 2006.
2. Worldental.org. The Most Traumatic Appointment in Dental Surgery - Tooth Extraction. Written April, 2008.
3. MayoClinic. Impacted Wisdom Teeth. Accessed July, 2008.https://www.mayoclinic.org/diseases-conditions/wisdom-teeth/symptoms-causes/syc-20373808
4. WebMD. Dental Health: Wisdom Teeth. Accessed July, 2008.
http://www.webmd.com/oral-health/guide/wisdom-teeth
5. IV (Intravenous) Sedation. Accessed October 2010. https://www.dentalfearcentral.org/help/sedation-dentistry/iv-sedation/
6. H. Ryan Kazemi. DMD. The Wise Guide to Wisdom Teeth Extraction: Making Engaged Decisions about Your Wisdom Teeth Extraction. 2010. Licensed under Creative Commons Attribution 3.0 U.S. License.
7. Heath Hendrickson. DDS. 2010.
8. Bodner L, et al. Characteristics of iatrogenic mandibular fractures associated with tooth removal: a review and analysis of 189 cases. Br J Oral Maxillofac Surg. 2010.
9. Javier Herce and et. al. Management of Impacted Third Molars Based on Telemedicine: A Pilot Study. Journal of Oral and Maxillofacial Surgery. Vol. 69. Issue 2. pages 471-475. 2011.
10. Parameters of Care: Clinical Practice Guidelines for Oral and Maxillofacial Surgery. Anesthesia in Outpatient Facilities. AAOMS ParCare 07. 2007.
11. S Kandasamy and DJ Rinchuse.
The wisdom behind third molar extractions. Australian Dental Journal. 54. pages 284-292. 2009. https://onlinelibrary.wiley.com/doi/full/10.1111/j.1834-7819.2009.01152.x
12. R. Liedholm, K. Knutsson, L. Lysell, and M. Rohlin. Mandibular third molars: oral surgeons' assessment of the indications for removal. Br J Oral Maxillofac Surg. vol. 37. pages 440443. 1999.
13. C.M. Dunne, C.A. Goodall, J.A. Leitch, and D.I. Russel. Removal of third molars in Scottish oral and maxillofacial surgery units: A review of practice in 1995 and 2002. Br J Oral Maxillofac Surg. vol. 44. pages 313-316. 2006.
14. Friedman JW. The prophylactic extraction of third molars: a public health hazard. Am J. Public Health. 2007. 97. pages 1554-1559.
15. J. W. Friedman. Friedman Responds. Am J Public Health. vol. 98. issue 4. pages 582 - 582. April 1, 2008.
| 
