|
Occipital Nerve Block
The information presented on this site is of personal opinion and consequently is slanted and biased and not based on proper scientific research. The information presented is NOT written by a dental expert. Further the information presented has NOT been subjected to peer review by experts to verify accuracy and data integrity.
I have had personal experience with an occipital nerve block in which the right occipital nerve block was blocked with lidocaine. This turned out to be very painful and a bad experience for me. Immediately following the block, I become weak and felt like I was going to faint. I had to lie down and receive an IV with fluids for 20 minutes. This is called a vasovagal reaction. After that I felt fine, but the block did not change my headache in anway. However, 2 weeks later I noticed constant severe nerve pain in my head, feelings of nerves moving around, and my neck being stiff. This has continued since I had it done in October of 2007 and I have been told is rare and can take 6 months before it heals, if at all. Because of this I would proceed with caution when considering an occipital nerve block.
Update: It has now been 6 months and I am still in constant pain and feel like the occipital nerve is damaged as a direct result of the nerve block. I will periodically update as far as progress goes.
Update 2: It is still problematic after 1 year.
Update 3: It is still a problem and is now May 2009.
Update 4: Still a problem as of August 15, 2009.
Update 5: Still problematic as of December 8, 2010. Since it has been over 3 years the damage from the nerve block is likely permanent : ( .
Update 6: The nerve damage is still a problem as of October 14, 2015. The nerve damage appears to be permanent.
Update 7: The nerve damage is still a problem as of October 14, 2019. The nerve damage must be permanent.
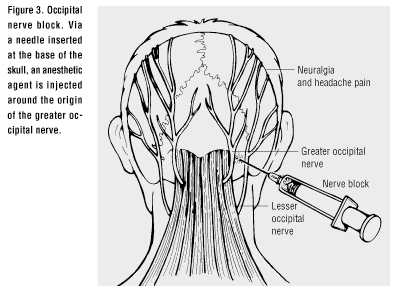
Occipital nerve block is a procedure where anesthetic agents (lidocaine and bupivacaine) are injected near the occipital nerve on the back of the head near the base of the skull on the side of the migraine headache. (The above figure shows the needle injected into the greater occipital nerve). Within five minutes after the nerve block, 60% of patients in a study had mild or no headache and 75% of patients had mild or no light sensitivity (photophobia). Allodynia (pain caused by a stimulus that normally does not produce pain, such as brushing your hair) also reduced quickly after the nerve block. Over half of patients in the study had no side effects. About 20% had pain at the injection site and about 20% experienced dizziness. The investigators concluded that greater occipital nerve blocks are safe and easy procedures that can be performed in the office and show results more quickly than oral triptan medications.
Another study focused on occipital nerve blocks using anesthetic agents plus a steroid medication. There was no statistically significant additional benefit when steroids were added to the treatment. I chose to elect to not use a steroid in the occipital nerve block I recieved due to the possibility of becoming aggressive or have other altering states.
The average duration of benefit in both trials was about four days. About 20% of responders still had total migraine headache relief one week after the injection.
Both trials were performed at the Thomas Jefferson University Hospital Headache Center in Philadelphia. With the small number of patients in both of these trials, it is difficult to know if these results would be noticed in a larger population. If an individual has true occipital neuralgia due to pinching or entrapment of the occipital nerve, then occipital nerve block may be of long-term benefit.
It seems that the practicality of this treatment is also questionable. Many neurologists have not been trained in how to perform occipital nerve blocks. Also, if the patient responds to triptan medications or other oral "abortive" medications, then occipital nerve block may not be reasonable.
If a medication is developed that could be injected in the occipital nerve region to provide a long-term reduction in the patient's migraine frequency, then this treatment would likely become standard of care.
Updated October 14, 2019
References
1. Dr. Seth Haplea. Occipital Neve Block for Migraine Headaches. Accessed July, 2008.
| 
