|
TMJ
What is TMJ (Temporomandibular Joint Syndrome)?
The information presented on this site is of personal opinion and consequently is slanted and biased and not based on proper scientific research. The information presented is NOT written by a dental expert. Further the information presented has NOT been subjected to peer review by experts to verify accuracy and data integrity.
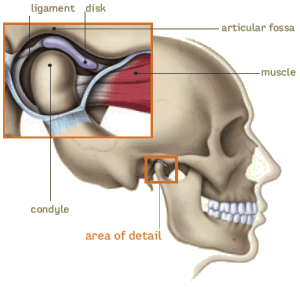
Temporomandibular joint and muscle disorders refer to a complex and set of conditions that can cause pain in the area of the jaw joint and associated muscles and/or problems using the jaw. Both or just one of the TM joints may be affected. This can affect a person's ability to speak, eat, chew, swallow, make facial expressions, breathe, cause head and neck pain, a jaw that is locked or difficulty to open, and popping/clicking noises. The TMJ is a hinge and gliding joint that is the most constantly used joint in the body.
Temporomandibular joint and muscle disorder has been reported of occuring in 5% to 12% of the population with a prevalence higher among younger people. [4]
The potential for TMJ problems exists in practically everyone—80 to 90 percent of the population has a tooth-gearing discrepancy. And day-to-day activities expose us to the common triggering of at least some TMJ symptoms. The absence of major symptoms in the vast majority of people is a tribute to our neuromuscular system's ability to protect us.
When a typical dental patient has a TMJ screening and is told that the potential for problems exists, this doesn't mean that the potential will ever be activated. The information simply lets the person know that if any of the mysterious symptoms of TMJ begin, the condition should be investigated.
TRAUMA AS A TRIGGER
Some of the triggers for TMJ are dramatic. A large number of patients seeking evaluation for TMJ can trace the onset of symptoms to some kind of trauma. Car accidents, sports injuries, a blow on the head or face, surgery, or loss of teeth can all trigger TMJ symptoms in susceptible people. Many other people suffer these traumas and do not become symptomatic. We don't know why some people will be pushed over the edge into symptom manifestation.
A common kind of trauma is automobile accidents. Even when an injury isn't terribly serious, a TMJ-susceptible person can become symptomatic. In a whiplash injury, the muscles in the neck are jarred and pulled suddenly, often causing severe stress. Sometimes the immobilizing collar that whiplash victims wear triggers symptoms. The collar pushes the lower jaw into the upper jaw and forces the lower jaw into a position that may be so unnatural that the external pterygoid muscles either go into spasm or increase their spasm.
Some people who seek a TMJ evaluation suffer an injury long before they actually seek help for their problems. At first the symptoms they experienced may have been minor, and it is assumed that they will eventually go away. For many fortunate people, they do, but for others, once the spasm cycle begins, it becomes established and doesn't go away on its own. For these people, the search for help begins when the discomfort seems to have no rhyme or reason and doesn't subside. They can trace their symptoms to some event, but they are told there is no apparent reason for the connection, especially if the injury sustained has healed normally.
Keep in mind that any kind of trauma can trigger TMJ. One patient could trace the beginning of his symptom cycle to a mugging. His attacker hit him in the face. He had no broken bones, but the blow was enough to cause symptoms, which included extremity numbness, neck and shoulder pain, intermittent middle-ear symptoms, and mild headaches. At first these symptoms were mild and infrequent, but gradually they became more severe.
Other people who have sustained trauma to the head and face will experience symptoms for a time, but gradually the symptoms disappear. The body can break this cycle of painful spasm on its own, and people forget these episodes ever occurred. The body's ability to heal is amazing, and more often than not, the TMJ symptoms triggered by trauma will eventually subside.
LOSS OF TEETH
Loss of teeth can trigger TMJ symptoms, although it may take years for this to happen. Whenever a tooth is lost, the teeth around it drift to fill the space. This changes the gearing scheme. Sometimes the body can accommodate the change, and no adverse affects are felt. Other times, a change, even a very subtle one in the gearing of the teeth, can trigger symptoms. Remember too, that even a minute gearing problem can cause severe symptoms. Yet some people walk around with severe gearing problems and no symptoms. We simply don't know why some people are especially susceptible to muscle spasms.
DENTISTRY AS A TRIGGER
Dentistry itself can trigger problems. Restorative work, as previously described, can trigger symptoms in patients who never experienced them before. A particularly sensitive patient can first experience TMJ symptoms during a period when much dental work is done. For some people, the stress of keeping the mouth opened wide is enough to make the muscles go into painful spasm. Numerous patients have reported this phenomenon. Something as minor as opening the mouth to bite into a large sandwich is enough to give some people a headache.
Patients will sometimes say that they knew, usually unconsciously, that certain activities put stress on their jaws. Sometimes they simply call it an "odd feeling" in the jaw when they have yawned widely, lifted weights, or started a jogging program. Some people let their mouths stay in a relaxed, slightly open position when they jog; others clench and even grind while they jog. If you wish to jog and you also experience even minor TMJ symptoms, try to stay in the more relaxed group rather than join the "clenchers."
My Experience
I remember hearing a noise whenever I would open or close my jaw all the way ever since I was in high school. I never had any pain associated with this clicking/popping noise, but it was there, and other people could hear it as well, especially at the dinner table. I thought it might have had something to do with having braces in middle school, and I spoke to my dentist about it. He told me he had the same thing. I never did anything further untill I started to suffer from a severe headache after the wisdom teeth were removed.
I wanted to explore all possibilites that could have been causing my headache and thus got a refferal from my dentist to a tmj specialist. When I visited with him in July of 2006, I told him my story while he inspected my teeth and bite. He told me that my headache was not a result of TMJ. However, he also told me that by the way a few of my teeth looked, he thought I clenched during the night. He thus wanted to make me a nightguard to wear to prevent me from clenching during the night. I agreed and had it fitted and made for my upper teeth. I then proceeded to wear the night guard almost every night over the next year.
The following summer I was still suffering from 24/7 head pounding and had been exploring many options. I heard from two seperate licensed massage therapits who both practiced craniosacral therapy (one working for a dentist and the other formerly a dentist and TMJ specialist as well) that an upper appliance restricts the craniosacral fascial system. Thus, I wanted to find a new TMJ specialist to see.
This time around, I was reffered to a much more experienced TMJ doctor. I explained to him my history and how my jaw has been popping/clicking whenever I open it all the way for many years. He told me that 1/3 of the population has popping/clicking whenever they open and close their jaw. He deals with patients who suffer from actual temporomandibular joint problems such as difficulty opening and closing the jaw, the jaw becoming locked, and lots of pain in the jaw. Further, the doctor explained to me that there was no need to wear a bite split at night.
Updated December 16, 2011
References
1. TMJ Syndrome. eMedicineHealth.
http://www.emedicinehealth.com/temporomandibular_joint_tmj_syndrome/article_em.htm
2. National Institute of Dental and Craniofacial Research. National Institutes of Health. Prevalence of TMJD and Its Signs and Symptoms . http://www.nidcr.nih.gov/DataStatistics/FindDataByTopic/FacialPain/PrevalenceTMJD.htm Accessed February 11, 2011.
| 
